December 20, 2022
We finally have the text of the (federal) omnibus budget bill that is expected to pass this week on The Hill in Washington, leaving us more assured than ever that the federal government will not be shutting down the government for the holidays. See below for that update and others.
But before we go there, please note that NY Democrats in the state Senate will retain their supermajority with the victory of incumbent John Mannion in central New York. Mannion secured his re-election by 10 votes after a recount and court battle in the 50th Senate district.
Mannion’s victory gives Democrats enough votes to maintain a supermajority in the 63-member chamber. Democrats in the state Assembly are also keeping their supermajority into 2023. Mannion was first elected to the state Senate in 2020.
FEDERAL UPDATES:
Federal Budget Deal: Last week, lawmakers announced there was finally a topline deal on the omnibus bill to continue to fund the federal government. Congress voted themselves an extension for a week (this week) to finish the bill.
We now have the text of the bill here: https://www.appropriations.senate.gov/imo/media/doc/JRQ121922.PDF. The bill dropped at around 2am this morning and now the Members will be busy moving it through the process for passage, starting with the motion to proceed later today. There are some important health care wins in the bill:
- Increased Medicaid funding for the territories--remember than in the territories, Medicaid is a block grant, not an entitlement, so it has to be reauthorized for funding every year by Congress. The agreement continues the 76 percent rate the federal government has been paying to match Puerto Rico’s Medicaid dollars for five years, as well as the higher limit on the money the federal government can put toward the island’s safety net program. For the rest of the territories, it permanently extends the federal match rate at 83 percent. This funding will prevent cuts that would have been required without it.
- Medicaid Reductions: The pandemic-era Medicaid rules tied to the Public Health Emergency (PHE) are due to expire next year and this bill includes more details on how states may proceed. A key rule was MOE (Maintenance of Effort), which prevented states from kicking people off their coverage even as they took on more enrollees. In the omnibus bill, states will be able to start reevaluating who is still eligible for the safety net program beginning in April — a key priority for Republicans. There will be guidance and guardrails over how states can reduce Medicaid rolls– such as requiring states to attempt to contact beneficiaries before they dis-enroll them from the program. The legislation gradually phases out the 6.2 percent funding bump states received for not touching their Medicaid rolls amid the pandemic.
- Maternal Health Extension: The legislation allows states to permanently extend Medicaid coverage for new moms for 12 months and prohibits children from getting kicked off Medicaid or the Children’s Health Insurance Program for a continuous 12 months, even if their family’s income changes.
- Provider Cuts in Medicare: these are cuts that are scheduled to go into effect every so often and which doc and hospital associations aggressively lobby against. The package partly fends off a nearly 4.5 percent cut to doctors’ Medicare reimbursement with the cut growing larger over the next two years. The AMA had lobbied Congress hard to avert the cuts in their entirety. Additionally, Congress extended the ability to qualify for a bonus payment for providers to participate in new ways of testing how Medicare pays for care for one year. However, lawmakers reduced the amount of the incentive from 5 percent to 3.5 percent.
- Telehealth: Emergency powers during the pandemic allowed telehealth to boom. But such policies were slated to go away roughly five months after the public health emergency for the coronavirus ends. Lawmakers are extending those Medicare telehealth flexibilities through 2024.
- Here’s the fact sheet on how much money the health agencies are getting.
- Here is the announcement from the Senate Appropriations Committee – scroll down to see links to separate summaries for each subcommittee area, etc.:
Read more here:
The Hill: Congressional negotiators roll out sweeping $1.7 trillion funding bill
Politico: 12/20/2022
CONGRESS BRINGS PRESENTS TO SOME, COAL TO OTHERS — Leading lawmakers unveiled a $1.7 trillion year-end spending bill early Tuesday as they raced to pass the sprawling package by week’s end, with federal cash expiring at midnight on Friday. The so-called omnibus includes nearly $119 billion for veterans’ care, a 22 percent increase, according to the office of Senate Appropriations Chair Patrick Leahy (D-Vt.).
What else: The spending package includes a deal that saves the government billions by ending pandemic era-Medicaid policies and directs some of the saved dollars toward giving low-income moms an extended coverage period on Medicaid in states that don’t already offer it.
— The deal includes language to extend hospital at-home waivers for two years, running through the end of 2024, POLITICO’s Ben Leonard reports. The waivers, established in November 2020, allow hospitals to treat some emergency department and inpatient hospital patients from their homes. The move was aimed at expanding hospital capacity as health care organizations were slammed with Covid-19 patients. The extension is one of several wins in the omnibus for those who favor expanding virtual care. Lawmakers also proposed a two-year extension of Medicare telehealth waivers as well as a provision enabling high-deductible health plans to offer telehealth appointments to subscribers before they’ve hit their deductibles.
— Ben also notes that lawmakers decided to sustain a ban on using federal dollars to craft unique patient IDs meant to pair patients with their health records. Close to 120 groups including AHIP, EHR vendors Epic and Cerner, and other industry groups pushed appropriators this spring to end the ban, along with AHIMA, HIMSS and CHIME.
— Physicians, who faced a 4.5 percent cut in Medicare rates in January, get a bit of a reprieve in the package. The new language would cut rates by 2 percent in 2023, and then 3.25 percent in 2024. Jack Resneck, the president of the American Medical Association, said in a statement that the move endangers the financial viability of some practices and threatens patient access.
“This 2 percent following two decades of flat payment rates will have consequences on health care access for older Americans,” he said in a statement. “High inflation compounds the threat to practice viability because physicians are the only Medicare providers without annual inflation-based updates.”
— Meanwhile, Sen. Bob Menendez said in a statement that he helped secure more funds for Puerto Rico’s Medicaid program to stabilize the territory’s health care system and improve the quality of care for residents. “I am proud to have secured this 76 percent FMAP reimbursement level over five years that will provide Puerto Rico with federal dollars that will enable the island to make critical investments that will help stabilize their health care system, retain health care providers, and improve access and quality of care for all of its residents,” he said in the statement.
The Senate is expected to act first on the spending package in the coming days, seeking a time agreement that would allow the bill to pass before Thursday night and sending it to the House. Any senator could hold up that deal in exchange for amendments or concessions. Senate Minority Whip John Thune said Monday that he expected conservatives to push for an amendment related to stripping out earmarks — or projects in lawmakers’ home states.
What senators were saying: Sen. Ron Wyden (D-Ore.) told Alice Miranda Ollstein he was confident the final bill would include policies that made “substantial concrete headway” on several health issues. “We made progress with respect to the areas of telemedicine, postpartum coverage and Medicare. You can question if this change or that is appropriate, but the reality is this is significant headway compared to the status quo that we were dealing with,” he said.
Sen. Roger Marshall (R-Kan.) said that while there were “some victories” in getting provisions from the PREVENT Pandemics Act into the text, he was disappointed that his bill to create a 9/11-style commission to investigate Covid-19 won’t be included. “Every layer of the onion that we peel back on the origins of Covid, we find that there’s more to it,” he said. “It’ll take a huge effort to really get to the truth.”
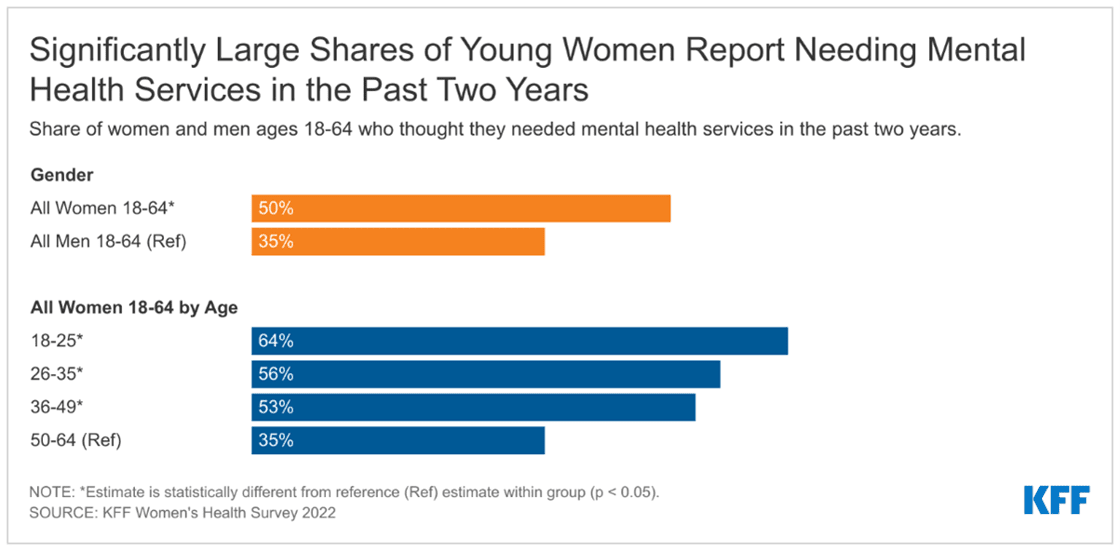
New Report: A new KFF report shows that more women need mental health services than ever but many are not able to get them.
See below for the report.
Large Shares of Women Report Needing Mental Health Services but Many Don’t Get Them: An analysis of 2022 KFF Women’s Health Survey (WHS) data finds that although large shares of women report needing mental health services over the past two years, a significant percentage did not access services they felt they needed. Fifty percent of women ages 18-64 say they needed mental health services in the past two years (including 64% of women ages 18-25), but only half of these women obtained an appointment, which may suggest unmet mental health care needs. Read the report.